Participate - Public Health Wales (Wrexham Maelor Hospital)
This site is recruiting participants from North Wales Area
Comparing COVID-19 Booster Vaccinations (COV-BOOST) - Omicron Variant Fourth Dose Booster
Please note : This site is not currently recruiting
What is the purpose of this research trial?
There are now a number of vaccines that have been approved in the UK to prevent COVID-19 and other vaccines that are still in UK clinical trials, which may be approved later in the year. Millions of people have now received their first 2 vaccinations, which we call a “prime-boost” course as well as a third dose booster vaccine. There were 2 vaccines used by the NHS to deliver an initial prime-boost during the first part of the NHS immunisation campaign: ChAdOx1-nCov19 (commonly known as the “Oxford vaccine” or ‘AstraZeneca Vaccine’), and BNT162b2 (commonly known as the “Pfizer vaccine”). The Omicron variant is now the most common variant of the virus which causes COVID-19 (SARS-CoV-2) in the UK, and due to mutations on its spike protein it is more capable of evading the immune response generated by existing vaccines against COVID-19 than previous variants. Two doses are thought to provide very little protection against infection (although they do provide good protection against severe disease), however three doses provide much improved protection against infection and severe disease or death. We also know that protection against infection wanes over a period of months following vaccination.
It is currently unknown whether providing further doses of existing COVID-19 vaccines (such as BNT162b2, the Pfizer vaccine) would produce better immune responses against the Omicron variant, or other variants of SARS-CoV-2 (such as Delta), or whether giving updated vaccines which are designed to help the body recognise the Omicron variant spike protein (such as mRNA-1273.529) would provide superior protection.
This study is trying to determine the side effect profile, safety and immune response of giving a different 3rd fourth COVID-19 vaccine booster doses of BNT162b2 (Pfizer) and mRNA-1273.529 (Moderna) to people who have previously received 3 doses of COVID-19 vaccine. We will be enrolling men and women aged 30 years or older who have received 3 doses of COVID-19 vaccine (with the third dose being either BNT162b2 or mRNA-1273) and are at least 3 months (84 days) after their third dose.
What are the vaccines against?
These vaccines are against the coronavirus SARS-CoV2 that causes the disease COVID-19.
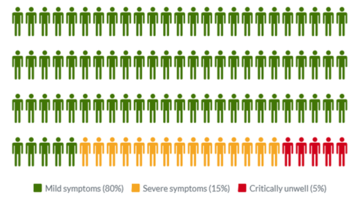
Common symptoms of COVID-19 include fever, tiredness, dry cough, and changes to taste and smell. Whilst about 80% of infected people have no or mild symptoms and will recover from the infection without needing special treatment, approximately 10-15% of cases (2-3 in 20) progress to develop severe symptoms, and about 5% (1 in 20) become critically ill.
There are some treatments that have been shown to be effective in reducing the severity of disease and the risk of death; but at present there is no cure. Older people and those with underlying medical conditions are more likely to develop serious illness. It has also been seen that people of some ethnic groups (Black and Asian) might be at a greater risk of severe illness. Some people also have symptoms that last a long time after they have recovered (commonly referred to as “long-COVID”). This is why effective vaccines are so important.
Am I suitable to take part?
Adults who are aged 30 years or older who have had 3 doses of a COVID-19 vaccine (with the third dose having been mRNA1273 or BNT162b2) and are at least 3 months (84 days) since their third dose are eligible to take part, providing that they have not previously tested positive for COVID-19 on a PCR, lateral flow, or saliva LAMP test. In order to participate in the study:
- You must be willing to tell the trial staff about your medical history, and you may be asked to allow the trial staff to check this with your General Practitioner (GP). Bear in mind that we would also notify your GP if you joined the trial (even if we did not need to check your medical history with them in advance).
- If you are able to become pregnant you must be willing to practice continuous effective contraception during the first 3 months of the trial and have negative pregnancy tests on the day of vaccination
- You must agree not to donate blood during the trial
For further details on why you could not take part in this study please see the Participant Information Sheet.
Summary of the study
We are studying the use of a new COVID-19 vaccine designed against the Omicron variant when given as a fourth dose booster, compared to a dose of BNT162b2 (the Pfizer COVID-19 vaccine). The Omicron variant has a large number of mutations to the “spike” protein on its surface, which is the protein most COVID-19 vaccines have used to train the body to recognise the virus which causes COVID-19 (SARS-CoV-2). This has made Omicron more effective at evading the immune response generated from existing vaccines. The pharmaceutical company Moderna which produced the mRNA-1273 vaccine for COVID-19, has adapted it and made a new vaccine (mRNA-1273.529) which produces a version of the spike protein which more closely resembles the one found on Omicron. We also know that giving a third dose of the Pfizer vaccine (BNT162b2) significantly increased the immune system’s ability to recognise the Omicron variant spike protein. This study is to evaluate the safety and side effect profile of giving a dose of mRNA-1273.529 compared to BNT162b2dose of the Pfizer COVID-19 vaccine to healthy adults, as a fourth dose COVID-19 booster, as well as assessing its impact on the immune response to the virus which causes COVID-19, called SARS-CoV-2different variants of SARS-CoV-2, including the Omicron and Delta variants.
Participants will be randomised to receive either a single dose of the BNT162b2 (Pfizer) vaccine or a dose of the mRNA-1273.529 vaccine. Participants will be “blinded”, meaning they will not be told which vaccine they have been given until after they have completed the study, or earlier in the event that having a fourth dose on the NHS app becomes a requirement for international travel. They will then complete a diary of their symptoms over the next 7 days, and any other adverse events which occur up to 3 months after having had the vaccine. There are four follow up visits over a period of 8 months to have blood tests to check for immune markers, and to check on the participants health.
What vaccines are being used in this study?
BNT162b2 (Pfizer/BioNTech) 30mcg
mRNA-1273.529 (Moderna) 50mcg
BNT162b2 (Pfizer/BioNTech): Common use under emergency provision
This is the vaccine commonly known as ‘The Pfizer vaccine.’ This is a messenger RNA (mRNA) vaccine. This vaccine uses a small amount of the genetic coding material (mRNA) of the SARS-CoV-2 spike (S) protein packaged inside very small fatty particles (lipid nanoparticles). When these are injected into your body, your cells take up these fatty particles, and then start producing the SARS-CoV-2 spike protein. Your immune system then “sees” these spike proteins and makes a protective immune reaction against them. The original mRNA that has been taken into your cells is broken down within a few days and cannot be incorporated into your own genetic code.
This vaccine has been tested in more than 40,000 people worldwide and subsequently given to tens of millions of people, and has been shown to be both safe, and effective.
The vaccine does not contain a live version of the SARS-CoV-2 coronavirus and therefore cannot give you COVID-19. The potential side effects of these vaccines are discussed in more detail in the section ‘What are the risks of taking part in this trial’.
mRNA-1273.529 (Moderna): Undergoing phase II clinical trials
This is an adapted version of the vaccine commonly known as “The Moderna vaccine”. This is also a messenger RNA (mRNA) vaccine which works in a similar way to BNT162b2 (The Pfizer vaccine). The updated version has changed the mRNA coding to more closely resemble that which is found on the Omicron variant of SARS-CoV-2.
This vaccine is currently undergoing phase II clinical trials to assess its safety and immunogenicity against different variants of SARS-CoV0-2.
Participants will not know which vaccine or dose they have received until they have completed all visits on the study, or earlier if having a fourth dose on the NHS app becomes a requirement for international travel.
What are the side effects of these vaccines?
Common side effects
People very often have tenderness, pain, warmth, redness, itching, swelling or bruising or less commonly have a small lump in their arm where they have been vaccinated.
Other common systemic side effects
Some people can develop these symptoms after vaccination. They usually last for less than a week after you are vaccinated (more commonly 24-48hours afterwards).
- Fatigue
- Headaches
- Flu-like symptoms, such as high temperature, sore throat, runny nose, cough and chills
- Muscle aches
- Joint aches
- Feeling unwell (malaise)
- Feeling sick or nauseated or vomiting
Other less common side effects:
- Abdominal pain
- Decreased appetite
- Feeling dizzy
- Swollen lymph nodes (glands)
- Excessive sweating, itching skin or rash
These symptoms can be reduced by use of paracetamol around the time of immunisation and over the next 24 hours.
After immunisation with the BNT162b2 (Pfizer/BioNTech) vaccine, difficulty sleeping has been observed in fewer than 1 in 100 people, and weakness of the muscles on one side of the face has been observed in fewer than 1 in 1000 people.
Data from studies comparing mixed prime-boost regimes of COVID-19 vaccination (e.g. Oxford/AstraZeneca followed by Pfizer) have found this may increase the risk of side effects following the second vaccine. It is possible that by receiving a COVID-19 booster vaccine in this study which is different to your original prime-boost regime previous COVID-19 vaccines, this might increase the side effects following vaccination.
What are the advantages of taking part?
We anticipate that participating in the trial will mean that you gain some additional protection against the coronavirus. Most importantly, the information gained from the trial will make a valuable contribution to the pandemic response.
Are there any risks from taking part in the study?
In addition to the potential side effects of the vaccines outlined above, the blood samples taken in the study may cause slight pain and occasionally bruising. Please refer to the participant information sheet for full details of procedures and potential risks.
What will happen if I don’t want to carry on with the trial?
If, at any time, after enrolment, you change your mind about being involved with this trial you are free to withdraw without giving a reason. If you withdraw we would not usually perform any more research procedures; although occasionally we might need to offer you a follow up visit for safety purposes, for example for blood tests. You would not have to agree to this. Your decision will not result in any penalty. Unless you state otherwise, any samples taken whilst you have been in the trial will continue to be stored and used for research as detailed above. You are free to request that your samples are destroyed at any time during or after the trial. Your data would be managed as laid out in the section ‘What will happen to my data’. If you choose to withdraw from the trial, your standard medical care will not be affected.
What’s next?
If you would like to find out more, please read the Participant Information Sheet and if you are interested in taking part, please complete our pre-screening questionnaire.
Download the Participant Information Sheet (PDF)
Please note : This site is not currently recruiting
Complete the Pre-screening Questionnaire
For further details contact us on :




